by Richard K. Bernstein, MD, FACE, FACN, CWS
2007
Diabetes Solution
The recent ruckus over the drug rosiglitazone (Avandia) has been portrayed as another case of Big Pharma foisting a dangerous drug on the public while the overworked FDA can’t keep up.
Search Google for Avandia and Vioxx, and you’ll come up with more than three-quarters of a million hits, including ads from law firms ready to litigate.
There is an enormous difference between the two situations. In the case of Vioxx, it was alleged that otherwise healthy people suffered sudden cardiac disease and death after using the pain reliever. This new study, published in the New England Journal of Medicine on May 21, alleges that Avandia causes an unacceptable rise in risk of heart attack. This—at least from the evidence presented—is hard to believe.
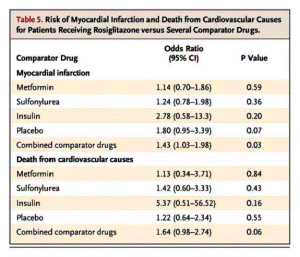 From The New England Journal of Medicine, 21 May, 2007
From The New England Journal of Medicine, 21 May, 2007
There are several ways to read the statistics that “support” this study.
Those in the Avandia meta-study were not only diabetics, but diabetics whose disease was initially out of control, with average blood sugar levels approaching three times those of non-diabetics and blood sugars at the ends of the studies undisclosed. The complications of diabetes—in this case heart disease—are caused by the prolonged elevation of blood sugars.
With a little math, we can easily conclude, for example, that metformin is about 4.75*-fold more likely to cause more cardiac deaths than insulin. We can also conclude that placebo is about 4.4**-fold more likely to cause more cardiac deaths than insulin. Which should lead us to the conclusion that since insulin is the most effective of these medications at lowering blood sugars, it is likewise more effective at reducing diabetic complications such as the risk of cardiac death.
The other drugs are considerably less effective in doing that job—but the sulfonylureas, while more effective than metformin or rosiglitazone in the short term, are problematic because they can over time, burn out remaining insulin-producing beta cells.
The real story behind these figures is that there are a lot of health care professionals who are not doing their jobs. Anyone with an initial (as in this study) HgbA1c level of 8.2 percent (equating to sustained average blood sugar levels of about 228 milligrams per deciliter) should be treated with insulin (and a low carbohydrate diet) since no combination of the other drugs can get such blood sugars normalized. The other drugs can have marginal effects in reducing blood sugar levels, but are not nearly so effective as insulin.
Blood sugars of diabetics can be normalized. The real ‘scandal’ is that very few health care professionals think that diabetics have the right to the same blood sugars as non-diabetics. They therefore leave their patients wide open to an unnecessary “potential for serious adverse cardiovascular effects.”




